Last Updated on March 12, 2024 by admin
Glucose, also known as blood sugar, affects our health and well-being. To put it simply, when we eat carbohydrates, our body breaks them down into glucose that is then used for energy or stored. Our levels should remain relatively consistent and low, and when they aren’t, it can be a sign of diabetes. High blood sugar levels are considered toxic, causing a range of health issues. For example, with type 2 diabetes, blood sugar remains high, putting individuals at greater risk for stroke, heart disease, and other issues. On the other end of the spectrum, when blood sugar levels are too low, a person can become hypoglycemic and even unconscious. Monitoring glucose levels is critical to managing diabetes, but it is no longer done exclusively by people with diabetes. With a Continuous Glucose Monitoring (CGM) sensors, people are able to monitor their glucose levels with ease.
An increasing number of people without diabetes are using technology to monitor their blood sugar levels. In 2019, an article in CNBC stated that “by 2025, everyone with diabetes will be tracking their blood sugar with devices called continuous glucose monitors, and it will be common for many people without diabetes to dabble in tracking, too.” So far, this proves to be correct. The sensor can be worn during daily activities like showering and exercising but expires after 14 days and will no longer be able to measure glucose levels and needs to be changed.
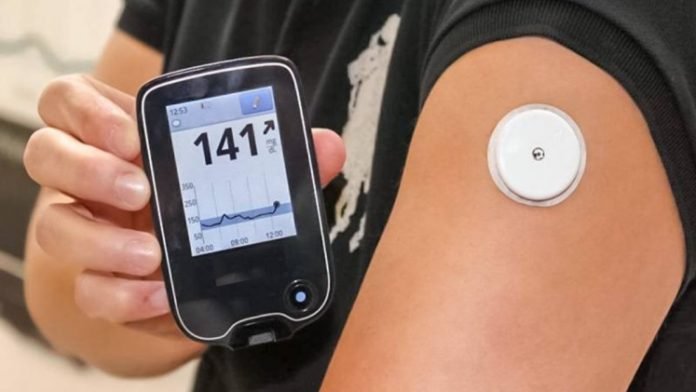
Initially developed for diabetics, a small, discreet sensor is attached to the back of your upper arm. It is painless and worn consistently for about two weeks, measuring interstitial fluids under the skin instead of blood. These measurements are then linked to an app on your phone, so you can quickly access your glucose levels in real-time.
Non-diabetic use of CGM sensors made headlines when journalist Lydia Ramsey Pflanzer from Insider wore a CGM Sensor to see if she could hack her performance by measuring her blood sugar. It’s done by “biohackers” as it helps individuals learn more about their body’s performance and how they react to certain foods.
Pflanzer, like other CGM-using biohackers, gained an plenty of insights into how her body responds to food and exercise. For example, she was surprised to learn that her blood sugar dropped significantly after having a beer with lunch. She also started to experiment – if she swapped out her morning breakfast of a banana with a granola bar, how would her body respond? As a marathon runner, she also wanted to use this information to better manage her glucose levels while running. Though Pflanzer did receive some backlash when she described her stable glucose levels as “boring,” many share her passion for understanding more about their glucose levels.
One of the reasons non-diabetics are looking to buy a CGM sensor is to discover how food and exercise affect them. Typically, if you do not have diabetes, you won’t experience volatile blood sugar levels; however, you will see that certain foods affect your levels more than others. For example, you may find your levels increase significantly after a workout, but the 3 pm candy you eat doesn’t make much of a difference. Having this understanding will allow you to adjust your routine and behaviors. For example, if you find out that a late afternoon sugary snack isn’t helping, you can cut it out and try to discover why else you may be getting sleepy mid-day. With a sensor, you may discover the energy slumps you experience are not related to glucose. Blood sugar levels can correlate to energy levels, but not always, and this is commonly misunderstood. For this reason, many reach for sugary drinks and beverages to boost energy when it may instead be a matter of hydration, hormones, or caffeine intake.
CGM sensors also provide users with insights into their sleep patterns. For example, many are intrigued by the blood sugar level patterns they see overnight that can be influenced by your bedtime routines like a late-night snack or an evening workout.
The actionable insights received from a CGM sensor help people without diabetes establish better lifestyle habits. Further, it can help those taking Metformin dial in on the proper dosage. People may also use a sensor when they have a family history of diabetes and are at greater risk. If you are concerned that you may develop diabetes, you can regularly monitor your glucose levels to see if there are any red flags that should be examined further.
When using a CGM sensor for biohacking purposes, you may find the data collected after 14 days is enough. That said, if you want to measure the effects of any behavioral changes you make, you may need more information and need a few sensors. After 14 days, you can apply a new sensor to continuing measuring your glucose.
According to the American Diabetes Association, there are recommended blood sugar levels for non-diabetics. For example, if your pancreas is functioning as it should and you are following a healthy diet and lifestyle, your levels should be between 70 and 130 mg/dl before a meal and less than 180 mg/dl two hours after starting a meal. The association also recommends that asymptomatic people who don’t suspect they have diabetes should still test their levels at least once every three years when over the age of 45.
Do you want to have more energy throughout the day? Feel more alert and focused? Sleep better or increase your athletic performance? By monitoring your glucose levels, you can discover ways to do this. AgelessRx.com, a telehealth subscription service that is focused on longevity therapies, sells CGM sensors. You can purchase one sensor (14 days) or three for more significant insights and up to 42 days of coverage. So, whether you are a self-proclaimed biohacker or just interested in your own health and well-being, a CGM sensor can provide you with actionable insights for optimal performance.
Read More: The Best and Worst Foods for Your Teeth
Apart from that, if you are interested to know about The Importance of HbA1c Test for Diabetes patients then visit our Health category.